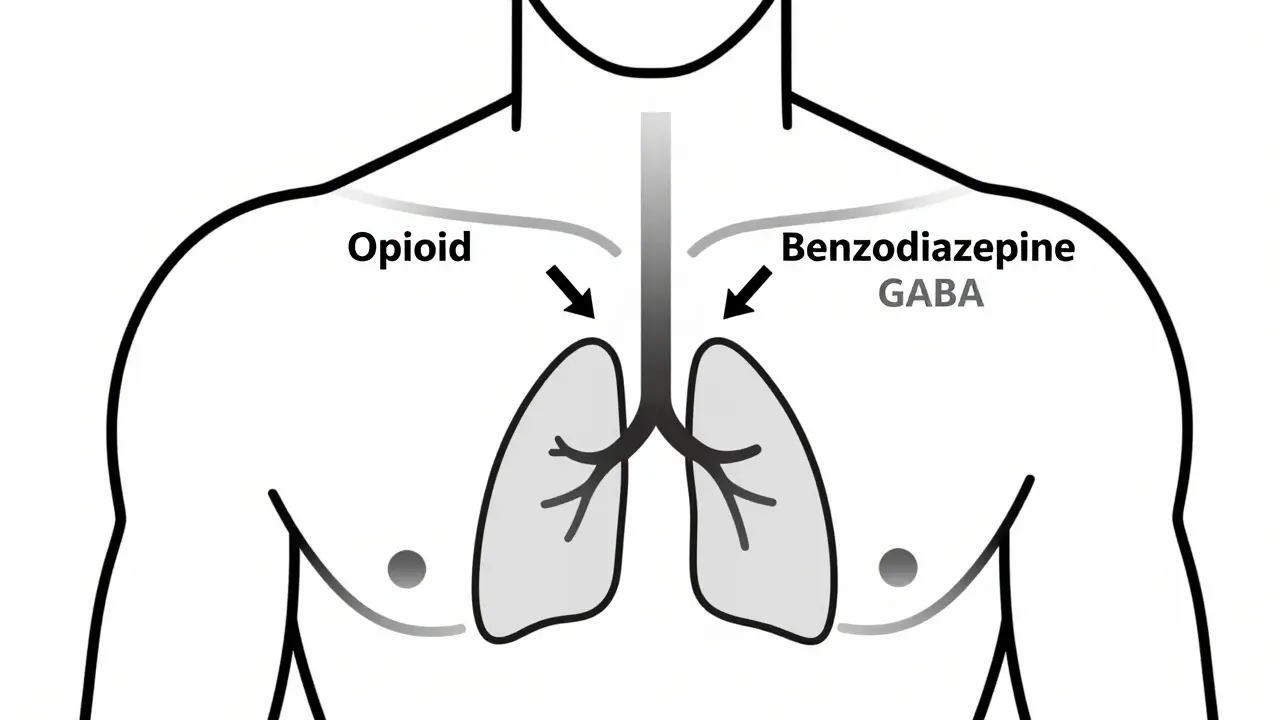
When you take opioids and benzodiazepines together, your body doesn’t just feel sleepy-it can stop breathing. This isn’t a hypothetical risk. It’s a deadly reality that kills hundreds of Americans every week. The combination doesn’t just add up; it multiplies danger. Both drugs slow down your central nervous system, but together, they turn a mild side effect into a life-or-death emergency.
Why This Combination Is So Dangerous
Opioids like oxycodone, fentanyl, and hydrocodone work by binding to mu-opioid receptors in the brainstem. These receptors control how hard and how often you breathe. When activated, they reduce the drive to inhale. Benzodiazepines like alprazolam, lorazepam, and diazepam work differently-they boost GABA, a calming neurotransmitter that suppresses brain activity, including the parts that keep your breathing regular. Alone, each drug can cause drowsiness or shallow breathing. Together, they create a perfect storm: your brain forgets to tell your lungs to work. Studies show that people taking both drugs are 10 times more likely to die from an overdose than those taking opioids alone. In 2020, 16% of opioid-related overdose deaths in the U.S. involved benzodiazepines. That’s not a small number-it’s nearly 1,000 people a month. And it’s not just illegal drugs. Many of these deaths happen because someone was prescribed both medications by different doctors, never realizing the risk.What Happens in Your Body
The danger isn’t just about feeling tired. When you take both drugs, your airway can collapse. Your tongue relaxes and blocks your throat. Your diaphragm stops moving properly. Your brain no longer responds to rising carbon dioxide levels-something that normally triggers you to gasp for air. In one study, 85% of people who took both drugs had oxygen levels drop below 90%, compared to 45% with opioids alone. That’s not just sleepy-that’s pre-arrest. There’s another hidden risk: metabolism. Some opioids, like fentanyl and methadone, are broken down by a liver enzyme called CYP3A4. Certain benzodiazepines, especially alprazolam, block this enzyme. That means the opioid builds up in your blood. A dose that was once safe can suddenly become toxic. You might not even feel it coming. One patient might take 5 mg of oxycodone and 1 mg of alprazolam for years without issue. Then, one night, their body can’t process the combo anymore-and they stop breathing in their sleep.Who’s at Highest Risk
You might think chronic opioid users are used to it. But that’s a myth. Tolerance to opioids doesn’t protect you from benzodiazepines. A person who’s been on painkillers for years can still overdose if they start taking Xanax for anxiety. The American Geriatrics Society warns that older adults are especially vulnerable. Their bodies process drugs slower. Their lungs are weaker. Their brains are more sensitive. That’s why the Beers Criteria lists this combo as potentially inappropriate for anyone over 65. People with sleep apnea, COPD, or asthma are also at extreme risk. Even if they’ve never had a problem before, adding a benzodiazepine can push them into respiratory failure. Emergency rooms see this all the time: someone with chronic back pain on oxycodone starts taking lorazepam for panic attacks, then ends up in the ICU after a night of heavy sleep.
What Doctors Are Supposed to Do
The FDA issued a formal warning in 2016 and strengthened it in 2019. They say: don’t prescribe these together unless there’s no other option. Even then, start low. Use the smallest dose possible. Monitor closely. Don’t combine them with alcohol or sleep aids. And never, ever prescribe opioid cough syrups to someone already on benzodiazepines. The CDC’s 2022 opioid prescribing guidelines say the same thing: avoid this combo whenever possible. Many hospitals now use electronic alerts that pop up when a doctor tries to write a prescription for both. One study showed these alerts cut dangerous co-prescribing by over 27%. That’s progress-but not enough. A 2021 study found that 15% of Medicare patients on long-term opioids were still getting benzodiazepines. That’s 1 in 7 people at risk.What You Should Do If You’re Taking Both
If you’re on both medications, don’t panic. But do act. Talk to your doctor. Ask: Is this really necessary? Is there a safer alternative for your anxiety? Could physical therapy, CBT, or non-addictive pain relievers replace one of them? Never stop either drug suddenly. Withdrawal from opioids causes sweating, nausea, and anxiety. Withdrawal from benzodiazepines can trigger seizures. Tapering must be done slowly under medical supervision. Your doctor can create a plan to reduce one drug at a time-usually the benzodiazepine first-while monitoring your breathing and mental state. Tell your family or caregiver what you’re taking. They need to know the signs of overdose:- Unresponsiveness
- Slow, shallow, or stopped breathing
- Blue lips or fingertips
- Snoring or gurgling sounds while asleep

Serena Petrie
March 15, 2026 AT 16:54Buddy Nataatmadja
March 17, 2026 AT 06:53mir yasir
March 18, 2026 AT 14:32Stephanie Paluch
March 19, 2026 AT 12:39tynece roberts
March 21, 2026 AT 00:19Hugh Breen
March 22, 2026 AT 20:16Byron Boror
March 24, 2026 AT 02:03Kelsey Vonk
March 24, 2026 AT 08:45Emma Nicolls
March 26, 2026 AT 05:34Richard Harris
March 26, 2026 AT 07:23Shruti Chaturvedi
March 26, 2026 AT 23:19Katherine Rodriguez
March 27, 2026 AT 19:27Devin Ersoy
March 28, 2026 AT 18:44Ali Hughey
March 30, 2026 AT 03:25